- Visibility 227 Views
- Downloads 35 Downloads
- Permissions
- DOI 10.18231/j.ijced.2025.012
-
CrossMark
- Citation
Disability profile of childhood and adolescent leprosy: A 10-year retrospective record-based study at tertiary care center
- Author Details:
-
Avanita Solanki
-
Neela Patel
-
Khushbu Modi
-
Niraj Dhinoja *
-
Twinkle Rangnani
Abstract
Aims and Objectives: Leprosy is a chronic granulomatous infectious disease in tropical countries. Children and adolescent with leprosy pose a great burden in society. Disability which develops in children and adolescent, have negative effect on social, personal and academic life. To break the chain of transmission in these patients we must find lacunae in disease development in those patients.
Materials and Methods: It is a retrospective record-based study conducted at tertiary care hospital. Case records for the period of 10 years (August 2010 to August 2020) were examined. All confirmed cases of leprosy who developed disability before, during and after taking MDT, were graded according to WHO disability grading (WHO 1988).
Results: Out of 568 patients diagnosed with leprosy, 61 (10.7%) patients developed disability, out of which 20 (32.78%) patients belonged to <15 years and 41(67.21%) belonged to 15-19 years. Male:Female ratio 2:1. 25 (41%) patients had positive family history and 20 (32.8%) patients had positive Slit skin smear examination for Acid fast bacilli. 25 (41%) patients had Multibacillary leprosy and 36 (59%) patients had Paucibacillary leprosy. 8 (13.11%) patients had type-2 lepra reaction while 6 (9.8%) patients had type-1 lepra reaction. Total 6 (9.8%) patients developed disability, out of which 2 (3.2%) patients had Grade 2 disability.
Conclusion: Leprosy in children is more important as it has great impact on child as well as family. Hence, regular close monitoring of child and adolescent with leprosy is required to avoid development of disabilities.
Introduction
Leprosy is a chronic granulomatous infectious disease caused by Mycobacterium leprae which is an obligate intracellular, acid-fast organism that tends to reside in cooler area of body like skin and peripheral nerves.[1]
Importance of detection of leprosy in children is that it represents community transmission of leprosy, lack of diagnosis of active cases and effectiveness of leprosy control program. The major concern is about development of crippling disabilities in children due to infiltration of tissue or nerve trunk by bacilli, which are enormously associated with psycho-social burden, limited academic and personal life; because it will remain for lifetime. Risk factors for developing disabilities in children includes late diagnosis, long term household contact, comparative low immune status, absence of obvious clinical signs and ignorance by parents due to social stigma. Adolescent age group is equally important as they are on the verge of their psycho sexual development and social maturation, they need to be protected from development of any disability.[2]
It is possible to prevent disabilities with early diagnosis and treatment which makes leprosy important cause of preventable disability and leading cause of permanent physical disability in the world.[3]
In 2019, among newly detected cases globally, 57% cases were from India. [4] During April 2019 to March 2020, total no. of new cases detected was 114,451, including 7859 (6.8%) child cases. Percentage of grade 2 disability among children in India on 31st march, 2020 was 0.8 while in Gujarat it was 0.[5]
Integration of NLEP with RKSK- Rastriya Kishor Surksha Karyakram (13-19 years) and RBSK- Rashtriya Bal Swasthya Karyakram (0-18 years) is to educate children and adolescents about leprosy and its possible outcomes as to early self-report and treatment.[5]
We aim to study disabilities in patients with childhood and adolescent leprosy, attending outpatient department.
Materials and Methods
A retrospective record based study was conducted at Department of Dermatology, Venereology and Leprosy at a tertiary care center where in case records of leprosy patients for the period of 10 years (August 2010 to August 202) were examined.
Inclusion criteria
Patients diagnosed with leprosy, <19 years of age (childhood leprosy i.e., <15 years and 15-19 years of age), based on clinical, histopathological and slit skin smear findings.
Exclusion criteria
Patients diagnosed as leprosy but lost to follow up.
Patients with disabilities, not due to leprosy.
Clinical images, slit skin smear results and histopathological findings including modified Fite Faraco staining reports were retrieved from the records. Patients diagnosed as having leprosy either paucibacillary or multibacillary, based on clinical and slit skin smear examination according to WHO classification. [6] Confirmed cases were further divided based on Ridley-Jopling classification. [7]
All confirmed cases of leprosy who developed disability before, during and after taking MDT, were graded according to WHO disability grading. [8]
All the necessary patients’ information (Demographic, clinical, laboratory parameters and disease related complication, that is disability including clinical photos) were obtained and analysed by SPSS 27 (Statistical Package for the Social Sciences 27) software.
The study was reviewed and approved by institutional review board. Confidentiality of all the data obtained from this study was maintained.
Results
During 10 years (August 2010- August 2020), out of total 568 patients diagnosed with leprosy, 61 (10.7%) leprosy patients were <19 years, out of which 43(70.49%) were males and 18(29.50%) were females. 20 (32.78%) patients lied below the 15 years age group while the maximum number of patients - 41 (67.21%) belonged to the 15-19 years. Patients were between 6-19 years with mean age of presentation 12.5 years and most common age group affected with disability was 15-19 years.
Out of 61 patients, 6 (9.83%) patients developed disability, of which 66.66% were males and 33.33% were females with male to female ratio 2:1.
Five (83.33%) patients in disability group and 23 (41.8%) patients among patients without disability had positive family history though not statistically significant. (p=0.052)
Out of 25 (41%) MB leprosy patients, 4 (16%) patients developed disability while in PB leprosy group, 2 (5.5%) patients developed disability out of 36 (59%) patients. Disabilities in patients with MB leprosy was more commonly seen in the 15-19 years age group (75%) while both <15 years and 15-19 years were equally affected with disabilities in the PB leprosy. (p=0.17)
Total 20 (32.78%) patients had positive Acid-fast bacilli (AFB) on slit skin smear examination out of which 5 (25%) patients had disability and 41 (67.21%) patients were negative for AFB, of which only 1 patient developed disability. This difference was statistically significant (p=0.0054).
Patients with type 2 lepra reaction developed disability more commonly than type 1 lepra reaction. Out of 5 patients with the history of type-1 lepra reaction, 1 (20%) patient developed disabilities while 4 (44.44%) patients with type 2 lepra reaction history developed a poor consequence. The most affected age group with disabilities among reaction patients was that of the 15-19 years (44.44%). (p=0.3) [[Table 1]]
|
|
|
<15 years |
15-19 years |
|
||
|
|
|
With Disability |
Without Disability |
With Disability |
Without Disability |
P value |
|
Age |
|
2 |
18 |
4 |
37 |
|
|
Sex |
Male |
1 |
10 |
3 |
29 |
|
|
|
Female |
1 |
7 |
1 |
9 |
|
|
Family/ contact |
Present |
2 |
11 |
3 |
12 |
0.052 |
|
|
Absent |
- |
14 |
1 |
18 |
|
|
MB/PB |
MB |
1 |
5 |
3 |
16 |
0.17 |
|
|
PB |
1 |
13 |
1 |
21 |
|
|
Skin Smear |
Positive |
2 |
4 |
3 |
11 |
0.0054 |
|
|
Negative |
- |
14 |
1 |
26 |
|
|
Reaction |
Type-1 |
- |
2 |
1 |
2 |
0.3 |
|
|
Type-2 |
2 |
2 |
2 |
3 |
Total 39 (64%) patients had history of presenting less than one year while 22 (36%) patients presented after 1 year. Total number of new cases (<15 and 15-19 years) had been decreased in second period. [[Table 2]]
|
|
|
<15 years |
15-19 years |
||
|
|
|
Period (Aug 2010-Aug 2015) |
Period (Aug 2015- Aug 2020) |
Period (Aug 2010-Aug 2015) |
Period (Aug 2015- Aug 2020) |
|
Duration of symptoms |
< 1 year |
9 |
4 |
20 |
6 |
|
|
>1 year |
4 |
3 |
11 |
4 |
|
Total |
|
13 |
7 |
31 |
10 |
Out of 6 patients, 33.33% 15-19 years suffered multiple disabilities while the rest – 66.66% had single disability with an equal ratio of 1:1 in the <15 years and 15-19 years age group. [[Table 3]]
|
Disability |
No. of patients (n=61) |
|
|
|
<15 years |
15-19 years |
|
No disability |
18 (29.50%) |
39 (63.93%) |
|
Single disability |
2 (3.27%) |
2 (3.27%) |
|
Multiple disabilities |
- |
2 (3.27%) |
6 patients developed disability, out of which 4 (66.66%) patients were 15-19 years and 2 patients (33.33%) were <15 years. In G2D, 2 (33.33%) patients of 15-19 years age group developed claw hand. 4 patients had already developed disability at the time of starting MDT, while 2 patients developed new onset of disability during MDT. [[Table 4]]
|
Treatment status |
< 15 years |
15-19 years |
||
|
|
Grade 1 disability |
G2D rate |
Grade 1 disability |
G2D rate |
|
Newly diagnosed |
1 |
- |
1 |
2 (40.00%) |
|
On MDT |
1 |
- |
1 |
- |
|
RFT (released from treatment) |
- |
- |
- |
- |
|
Total no. of patients |
2 |
- |
2 |
2 |
|
Site |
Disability |
<15 yrs |
15-19 yrs |
|
Hand |
Anaesthesia |
2 |
2 |
|
|
Claw hand |
- |
2 |
|
|
Ulcers |
- |
|
|
|
Resorption of digits |
|
|
|
|
Other |
|
|
|
Foot |
Anaesthesia |
|
2 |
|
|
Foot drop |
|
|
|
|
Ulcers |
|
|
|
|
Resorption of digits |
|
|
|
|
Other |
|
|
|
Eye |
Redness |
0 |
|
|
|
Blurring of vision |
0 |
|
|
|
Lagophthalmos |
0 |
|
|
|
Madarosis |
0 |
|
|
<15 years |
15-19 years |
||
|
|
Total no. of patients |
Patients with disability |
Total no. of patients |
Patients with disability |
|
Lepromatous leprosy |
5 (25%) |
1 (20%) |
14 (34.14%) |
2 (15.38%) |
|
Borderline lepromatous leprosy |
3 (15%) |
1 (33.33%) |
7 (17.07%) |
1 (14.28%) |
|
Mid borderline leprosy |
5 (25%) |
- |
7 (17.07%) |
1 (14.28%) |
|
Borderline tuberculoid leprosy |
3 (15%) |
- |
6 (14.63%) |
- |
|
Tuberculoid leprosy |
4 (20%) |
- |
7 (17.07%) |
- |
|
Pure neuritic leprosy |
- |
- |
- |
- |
|
Total |
20 |
2 |
41 |
4 |
|
Duration |
Total no. of patients |
No. of patients with disability |
||
|
|
<15 yrs |
15-19 yrs |
<15 yrs |
15-19 yrs |
|
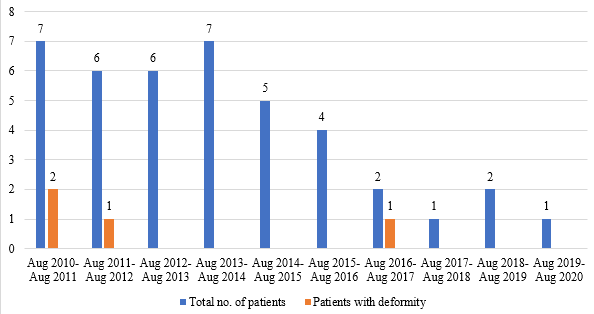
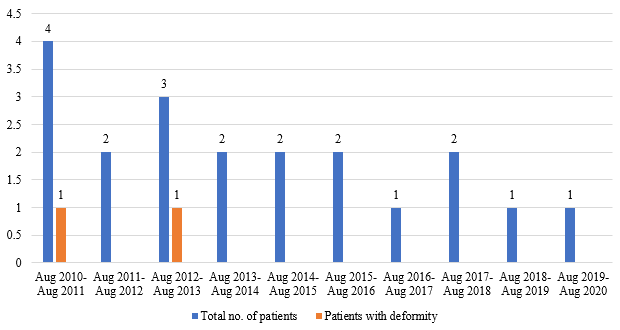
Aug 2010- Aug 2011 |
4 |
7 |
1 (25.00%) |
2 (28.57%) |
|
Aug 2011- Aug 2012 |
2 |
6 |
- |
1 (16.66%) |
|
Aug 2012- Aug 2013 |
3 |
6 |
1 (33.33%) |
- |
|
Aug 2013- Aug 2014 |
2 |
7 |
- |
- |
|
Aug 2014- Aug 2015 |
2 |
5 |
- |
- |
|
Aug 2015- Aug 2016 |
2 |
4 |
- |
- |
|
Aug 2016- Aug 2017 |
1 |
2 |
- |
1 (50.00%) |
|
Aug 2017- Aug 2018 |
2 |
1 |
- |
- |
|
Aug 2018- Aug 2019 |
1 |
2 |
- |
- |
|
Aug 2019- Aug 2020 |
1 |
1 |
- |
- |
Discussion
Leprosy elimination programmes have been moving along the spectrum from targets on reducing the prevalence of the disease to targets that emphasize on the decrease in the number of new cases with G2D for early detection and reduce transmission. [9] Disability can range from mere sensory impairment to gross paralytic and degenerative disabilities. Involvement of more than one body part such as hands, feet or eyes may be considered more severe than involvement of only one body part. [10]
During the study period total 568 patients were diagnosed with leprosy, out of which 20 (3.5%) were <15 years and 41 (7.2%) were 15-19 years, with children to adolescent ratio 1:2. Percentage of patients <19 years of age was 10.73%.
Most of our patients (67.21%) were 15-19 years and they were the major population with disability. Ramos et al found the similar finding. [11]
Boys were more commonly affected than girls with male: female ratio of 2:1 in 15-19 years age group. Same findings were proposed by Asia Anand J, [12] Lana et al, [13] Gitte et al [14] and Kar et al. [15] There was no much gender difference in <15 years age group.
Apart from long incubation period, boys especially of adolescent age group are more likely to have environmental exposure, engaged in work, inattention to relatively asymptomatic lesions of leprosy and associated stigma.
It is interesting to note that most patients in this study were in the lepromatous spectrum than in the tuberculoid spectrum in this study. One would expect more patients among the childhood and adolescent group to have BT leprosy. This might be due to poor nutritional and immunological status of affected age groups.
5 patients developing disability had positive family history/contact history, justifying longer duration of contact with untreated/ treated case. For example, one girl with tuberculoid leprosy had mother with lepromatous leprosy.
16% in MB group and 5.5% in PB group developed disability. This finding can be correlated with study done by Asia Anand J [12] while in studies done by Lana et al [13] and Kar et al [15] showed higher disability in MB group (34.5% and 24% respectively) than present study.
25% patients developed disability out of total smear positive patients and only one patient developed disability out of total smear negative patients, which was statistically significant. Kar et al [15] found similar finding in their study.
Above findings can be justified by higher bacillary load and more extensive neural involvement.
Patients with type-2 lepra reaction were commonly associated with disability than type-1 lepra reaction. This may be because type-2 lepra reaction was common in 15-19 years age group in our study and disability was common in 15-19 years of age.
4 (66.66%) patients had disability at the time of presentation while 2 (33.33%) patients developed disability during treatment with MDT. This finding can be related to delay in diagnosis of leprosy which leads to development of disability and need for effective leprosy program.
Among newly detected patients, Grade 2 disability was seen in 3.2% patients. Similar percentage of G2D was found in study done by Asia Anand J while kar et al [15] and Gitte et al[14] found a greater number of G2D, 10.5% and 17% respectively, which may be due endemicity of disease in that area.
There was no record of madarosis or other facial features of in spite of 19 patients with LL. This is may be probably because of the duration of the disease and early diagnosis and treatment with MDT.
While 2 patients had multiple disabilities and 4 patients had single disability. Most common part involved in disability was hand and common disability was loss of sensation ([Table 5]). Duration of symptoms was less than one year in most of the patients specially in adolescent age group ([Table 2]).
Most common type of leprosy in both the age group was lepromatous leprosy (29.5%), followed by mid borderline leprosy (19.67%), tuberculoid leprosy (18.03%), borderline lepromatous leprosy (16.4%) and borderline tuberculoid leprosy (14.75%). Disabilities were more common in borderline lepromatous leprosy followed by lepromatous leprosy and mid borderline leprosy.
In comparison to August 2010- August 2015, child and adolescent leprosy cases including patients with disabilities were less in number during August 2015- August 2020 ([Table 7]). It may be due to more awareness about the disease, early treatment seeking behavior of patients and easy availability of MDT.
Conclusion
Though leprosy has been eliminated from India since 2005, still children and adolescent leprosy cases are coming up in endemic and non-endemic aeras.
Children are at risk population because of late presentation, inadequate early case detection, neglect on the part parents to consult health system. Hence, early case detection, contact tracing, timely treatment is most important.
There are clear differences in the patient characteristics of children and adolescents but further study is needed to enable the interpretation of this study to larger population. We have found declining trend in total leprosy patients and patients with disability and low prevalence of childhood as well as adolescent leprosy as compared to other studies suggest, early identification of signs and symptoms of leprosy and reactions and their early treatment.
Reduction of stigma and motivating parents to bring their children to the hospital at the earliest sign of leprosy is of utmost importance in the present situation. Timely surveys and screening of school going children may identify early cases. To achieve this, more health care workers should be trained effectively to identify leprosy cases.
Conflict of Interest
None.
Source of Funding
None.
References
- Bhandari J, Awais M, Robbins BA. Leprosy. StatPearls [Internet]. 2024. [Google Scholar]
- Darlong J, Govindharaj P, Darlong F, Mahato N. A study of untreated leprosy affected children reporting with Grade 2 disability at a referral centre in West Bengal, India. Leprosy Rev. 2017;88(3):298-305. [Google Scholar]
- . World Health Organization (2005). Global Strategy for Further Reducing the Leprosy Burden and Sustaining Leprosy Control Activities. Plan period: 2006-2010. . . [Google Scholar]
- . Weekly epidemiological report. . 2020;95:417-40. [Google Scholar]
- . Govt. of India. National Leprosy Eradication Programme (2020). Directorate General of Health Services, Central Leprosy Division, Nirman Bhawan, New Delhi. . . [Google Scholar]
- . WHO Leprosy Elimination Group (WHO). 2000. Guide to eliminate leprosy as a public health problem [Internet]. . . [Google Scholar]
- Ridley D, Jopling W. Classification of leprosy according to immunity. A five-group system. Int J Lepr Other Mycobact Dis. 1966;34(3):255-73. [Google Scholar]
- . WHO Expert committee on leprosy. Sixth report. WHO technical report series 1988; 768. . 1988. [Google Scholar]
- . Regional Office for South-East Asia, World Health Organization. (2016). Global Leprosy Strategy 2016-2020: Accelerating towards a leprosy-free world. WHO Regional Office for South-East Asia. . . [Google Scholar]
- Patel N, Modi K. A cross-sectional study of deformities in patients of leprosy at a tertiary care center of Western India. Indian J Lepr. 2016;88:209-15. [Google Scholar]
- Ramos J, SO, Lemma D, Petros M, Ortiz-Martínez C, Tesfamariam A. Isabel Belinchón, Epidemiological and Clinical Characteristics of Children and Adolescents with Leprosy Admitted Over 16 Years at a Rural Hospital in Ethiopia: A Retrospective Analysis. J Trop Pediatr. 2018;64(3):195-201. [Google Scholar]
- Anand A, J. Profile of Disability in Children with Leprosy. Int J Sci Res Publ. 2018;5(10):1-4. [Google Scholar]
- Lana F, Fabri A, Lopes F, Carvalho A, Lanza F. Deformities due to Leprosy in Children under Fifteen Years Old as an Indicator of Quality of the Leprosy Control Programme in Brazilian Municipalities. J Trop Med. 2013. [Google Scholar] [Crossref]
- Gitte S, Sabat R, Kamble K. Childhood Leprosy in an Endemic Area of Central India. Indian Pediatr. 2016;53(3):221-4. [Google Scholar]
- Kar B, Job C. Visible deformity in childhood leprosy--A 10-year study. Int J Lepr Other Mycobact Dis. 2005;73(4):243-8. [Google Scholar]
How to Cite This Article
Vancouver
Solanki A, Patel N, Modi K, Dhinoja N, Rangnani T. Disability profile of childhood and adolescent leprosy: A 10-year retrospective record-based study at tertiary care center [Internet]. IP Indian J Clin Exp Dermatol. 2025 [cited 2025 Oct 06];11(1):84-89. Available from: https://doi.org/10.18231/j.ijced.2025.012
APA
Solanki, A., Patel, N., Modi, K., Dhinoja, N., Rangnani, T. (2025). Disability profile of childhood and adolescent leprosy: A 10-year retrospective record-based study at tertiary care center. IP Indian J Clin Exp Dermatol, 11(1), 84-89. https://doi.org/10.18231/j.ijced.2025.012
MLA
Solanki, Avanita, Patel, Neela, Modi, Khushbu, Dhinoja, Niraj, Rangnani, Twinkle. "Disability profile of childhood and adolescent leprosy: A 10-year retrospective record-based study at tertiary care center." IP Indian J Clin Exp Dermatol, vol. 11, no. 1, 2025, pp. 84-89. https://doi.org/10.18231/j.ijced.2025.012
Chicago
Solanki, A., Patel, N., Modi, K., Dhinoja, N., Rangnani, T.. "Disability profile of childhood and adolescent leprosy: A 10-year retrospective record-based study at tertiary care center." IP Indian J Clin Exp Dermatol 11, no. 1 (2025): 84-89. https://doi.org/10.18231/j.ijced.2025.012
